The temporal bone has five parts: squamous, mastoid, petrous, tympanic, and styloid process. The largest is the squamous part; it is flat and forms the temporal fossa. The pyramid-shaped petrous part is at the base of the temporal bone, and contains the inner ear. The tympanic part surrounds the external auditory canal.
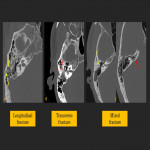
The traditional system of classification of temporal bone fractures is based on the relationship of the fracture line relative to the long axis of the petrous pyramid of the temporal bone and can be either longitudinal or transverse. Longitudinal fractures are parallel to the long axis and are more common (80-90%), resulting from temporoparietal trauma. Transverse fractures occur due to fronto-occipital trauma, and are perpendicular to the long axis of the petrous bone. Mixed fractures occur when elements of both are included. This classification is descriptive and does not correlate with clinical outcome or complications.
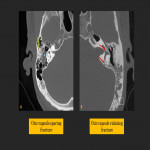
Other classification methods include assessment of otic capsule involvement, and can be classified as otic capsule violating or sparing. The otic capsule sparing type is more common, and correlates with conductive hearing loss due to injury to the ossicles. The otic capsule violating type is associated with sensorineural hearing loss, facial nerve paralysis, and perilymphatic fistula.
Although classification of fractures can be useful, it is essential to carefully identify injury to individual critical structures and associated complications for prompt management and prognostication. These complications include traumatic vascular injury, conductive or sensorineural hearing loss, facial nerve paralysis, peri-lymphatic fistulas, cerebrospinal fluid leak, etc. These specific areas and complications are discussed individually, and are part of the checklist when assessing temporal bone trauma.
External auditory canal
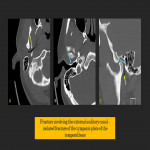
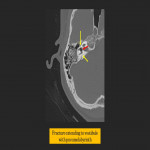
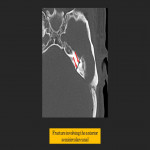
Fracture involvement of the external auditory canal (EAC) may present acutely with bloody discharge from the ear. The anterior wall of the EAC may be involved due to impaction of the mandibular condyle or through extension of a fracture line into the EAC. Due to its close relationship to the temporomandibular joint (TMJ), involvement of the EAC should prompt closer inspection of the TMJ. Left untreated, EAC fractures can lead to canal stenosis.
Ossicular injury
Ossicular chain disruption can be due to displacement or fractures. While conductive hearing loss can occur initially due to tympanic membrane rupture or hemotympanum, persistent conductive hearing loss after one month should raise suspicion of ossicular injury.
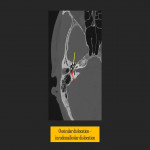
The five types of ossicular dislocation are incudostapedial separation, incudomalleal separation, incus dislocation, incudomalleal complex dislocation, and stapediovestibular dislocation. The most common type is the incudostapedial joint separation, and can be seen as a gap between the head of the stapes and the lenticular process of the incus. Stapediovestibular dislocation is due to disruption of the stapes footplate attachment to the oval window, resulting in possible internal or external dislocation of the stapes. It may be complicated by a perilymphatic fistula at the oval window.
The long process of the incus is most commonly involved in ossicular fracture due to lack of support, followed by the stapedial crura.
Perilymphatic fistula
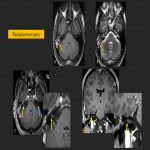
Perilymphatic fistula refers to an abnormal connection between the membranous labyrinth and the tympanic space. Patients may present with vestibular symptoms such as imbalance and vertigo with fluctuating sensorineural or mixed hearing loss. It is most commonly due to rupture of the oval or round window secondary to trauma. Although the offending fracture itself might be difficult to see, pneumolabyrinth in the correct clinical setting may suggest its presence. On MRI, post-contrast T1 weighted images may show segmental enhancement of the membranous labyrinth in the affected regions.
CSF leakage
CSF leakage is seen more commonly in otic-capsule violating fractures, particularly with involvement of the tegmen. Patients present with CSF rhinorrhea or otorrhea. It usually occurs in the first week after trauma and tends to close spontaneously. Prolonged leakage (over 1 week) increases the risk of meningitis.
Facial nerve injury
Injuries to the facial canal occur most commonly with transverse fractures, which should prompt careful interrogation of the course of the facial canal. When the facial canal is involved, 50% are associated with facial nerve injury. The most common sites are the labyrinthine portion and the geniculate portion. Facial nerve injury manifests as nerve contusion, edema, or transection.
Vestibular injury
The vestibule is involved in coordinating balance, and connects to the cochlea and semi circular canals. Injury to the vestibular apparatus can lead to vertigo.
Semicircular canal injury
The three semicircular canals contain sensory organs that respond to angular acceleration. They are positioned orthogonally to one another and connect to the vestibule. Similar to vestibular injury, semicircular canal injury can lead to vertigo.
Labyrinthitis ossificans
Otic capsule violating fractures may result in the normally fluid-filled cavities of the otic capsule becoming replaced by fibrous tissue, and eventually by bone. This is called labyrinthitis ossificans. Patients present with sensorineural hearing loss and vestibular dysfunction. Bone attenuation can be seen in the inner ear structures on CT, while MR shows loss of normal fluid signal intensity of the membranous labyrinth with enhancement on post-contrast images. The early fibrous stage is best evaluated by MR, seen as a loss of fluid signal.
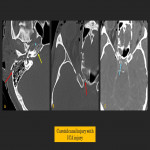
Carotid canal involvement
The carotid canal is in the petrous portion of the temporal lobe. 35% of fractures involving the carotid canal have associated ICA injury. Due to this, assessment of ICA by angiography is indicated in traumatic involvement of the carotid canal. Injury to the ICA can manifest as occlusion/thrombosis, pseudoaneurysm formation, dissection, transection or arteriovenous malformation.
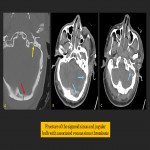
Jugular bulb and sigmoid sinus involvement
Similar to carotid canal fractures, fractures involving the jugular bulb and sigmoid sinus can lead to thrombosis or laceration of the internal jugular vein or sigmoid sinus. Acute venous thrombosis can demonstrate high density on unenhanced CT images, which should additionally raise suspicion. Sinus thrombosis may be complicated by venous infarcts, and laceration can lead to intracranial hemorrhage.